What are the challenges and approaches for AHP support and supervision north of the border? Are there any lessons for employers?
Gail Nash, NHS Education for Scotland's AHP Practice Education Programme Lead, explains how NHS Scotland enables AHPs to participate in meaningful supervision practice.
Background
The Allied Health Professions (AHP) Practice Education (PE) programme at NHS Education Scotland (NES) provides education and support for the AHP workforce across Scotland. The infrastructure spans 14 territorial boards and 2 national boards supporting a workforce of approximately 12,500 AHPs and healthcare support workers (HCSW).
The programme works within a multi-professional and multi-agency context, engaging closely with NHS Boards, the Scottish Government, HCPC, Scotland’s universities and colleges, social care and many other cross-sectoral partners and stakeholders, to support the workforce delivering patient care.
One of the practice education (PE) priorities in Scotland is AHP Support and Supervision. Following several high-profile inquiries within the United Kingdom (UK) into significant adverse care events, greater emphasis has been placed on ways in which staff are supported in the workplace (Department of Health 2012, The Mid Staffordshire NHS Foundation Trust Public Inquiry 2013, Andrews and Butler 2014, The Vale of Leven Hospital Inquiry 2014, Kirkup 2015). HCPC ‘Preventing small problems becoming big problems’ (2014) and research commissioned by HCPC (2019) both highlight the importance of quality supervision being key, not only supporting professional development, but also staff health and wellbeing and identifying risks early.
Implementing AHP Support and Supervision in Scotland
In 2018 a joint statement from the Allied Health Professions (AHPs) in Scotland/NHS Education for Scotland provided guidance that 'all AHP practitioners, irrespective of their level of practice or experience, should have access to, and be prepared to make constructive use of supervision.' This statement offered principles and guidance to support the provision of supervision for all AHPs and AHP HCSW working across health and social care in Scotland. Hear from our Chief AHP Officer, Carolyn McDonald, here.
Alongside this a national survey was conducted which highlighted the following challenges faced by the workforce:
- Supervision practice was very disparate and not uniformly available
- Staff were often unclear about what should be covered in supervision
- Lack of clarity about the type, mode, frequency and how to record supervision
- Staff did not feel confident in their role as a supervisor or supervisee
- Staff were unsure where to access education and resources to support their practice
In response, the NES AHP PE team set up a national working group (NWG) to support implementation of the position statement’s principles. It also expanded its capacity to design, deliver and evaluate evidence-based education to enable AHPs to participate in quality and meaningful supervision practice.
Governance
To ensure governance and assurance around this work the following measures were adopted:
- An AHP advisory group supported by AHP Directors Scotland group and AHP Federation Scotland group was established. This group ensures delivery of this workstream in alignment with the principles in the position statements (2018), current research (HCPC 2019) and those identified in the NES literature reviews.
- Infrastructure: Funding specific posts has been critical to the delivery of the project as well as utilising the existing networks and developing a sustainable model. A quality improvement approach to the development and implementation, including facilitator development via a ‘train the trainer’ approach; workshop design; user group testing; resources and Turas learning site (the national learning platform for health and social care staff in Scotland) development; and aligning local policies / guidelines to the principles in both position statements enabled the ability to deliver at pace and scale.
- Learner support has been provided by the AHP Practice Education Leads (PELs) in each board area.
Quality, performance, and impact
The methodology and key achievements to date have been captured in an infographic and summarised in a poster.
Practical considerations in implementing supervision
Some questions we have heard from employers:
Where do we start?
It is important to have support from directors and leadership teams to promote the importance of supervision for the workforce as a whole. Consider what is already happening within your area. Can you build upon this? Do you have staff who are enthusiastic about this and can lead on it? Here are two examples from practice:
- Lorna Darrie, Physiotherapist Supervision perspectives - Physiotherapy on Vimeo
- Rebecca McFadyen, Speech and Language therapist - Supervision perspectives - Speech and Language Therapy on Vimeo
Who is to receive supervision?
All staff within the workforce should engage in support and supervision. This includes from HCSW to AHP managers. Staff may need different supervisors for different roles within your organisation. For example, a manager who is also a clinician may need time to reflect on management projects as well as time to reflect and develop skills within their clinical role.
How do we identify supervisors?
It is important that supervisors feel confident and supported in their role. Within the HCPC article ‘The characteristics of effective clinical and peer supervision in the workplace: a rapid evidence review’ (2019), it identified that the supervisor/supervisee relationship is important in the success of the supervision and therefore staff need to feel confident and supported within this role. In addition, it is important to consider that supervisees should be allowed to choose their clinical/practice supervisor. How could this work within your service? For example, is it worth creating a list of supervisors and time they can give to sessions?
How can supervision be delivered?
There are many ways of delivering supervision. This can be done on a 1:1 basis, group supervision, peer group supervision, triad, or a combination. It is important to consider the needs of your staff group and look at how they will get the best from these sessions in terms of their development and support.
- Here is a short video showing a group supervision session in action. https://vimeo.com/746562992
What training do staff need?
Providing training for all staff members to help with engagement within the process is important. This can be used as a launch of supervision within your area. It raises awareness of the benefits of supervision as well as providing training for supervisors to improve their confidence in providing sessions. We devised two webinars and an interactive skills session for all staff. In addition, we have developed resources which are available on TURAS learning site. What training resources do you already have?
Is there a particular model we should use?
There are numerous supervision models within literature, the one most widely quoted in literature is Proctor’s model (1987). Within our sessions we discussed a general model detailing 4 types of supervision, all underpinned by Proctor’s model.
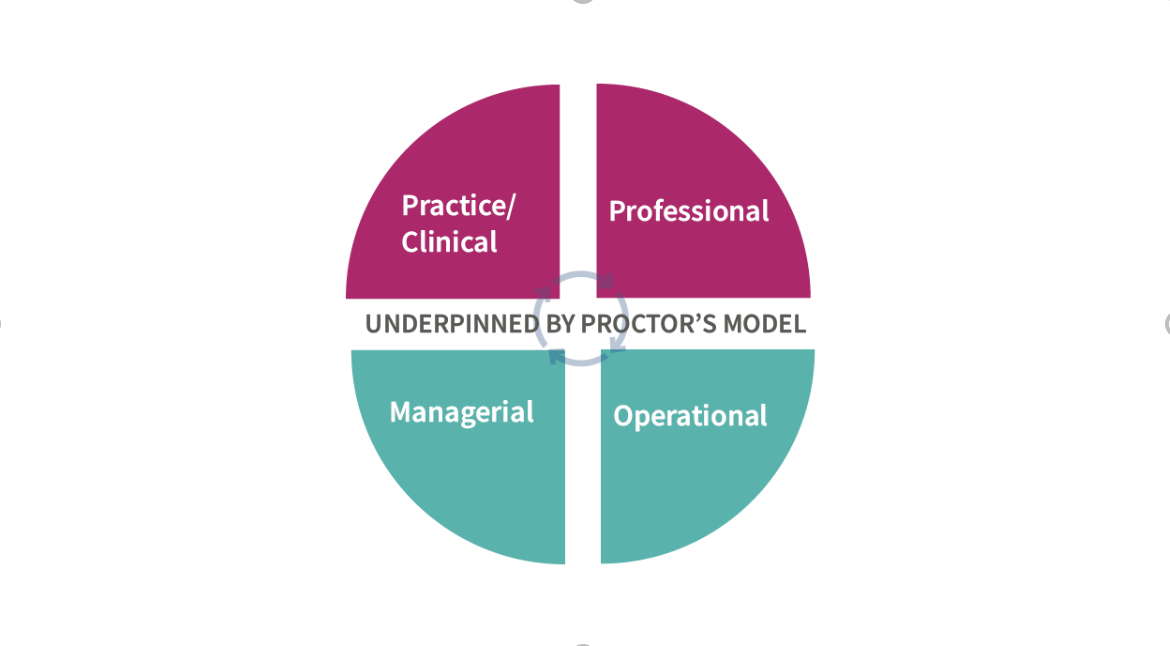 Diagram 1
Diagram 1
The four types include practice/clinical and professional (these are often combined and called clinical supervision); managerial and operational are also frequently combined and referred to as line management supervision.
How often should staff receive supervision?
There are no set timescales for frequency of sessions but a general understanding that supervision should be regular and cover the four types of supervision described above (Diagram 1). The Scottish position statement provides guidance on minimum of 4 times per year. Data from the 2018 National Survey told us that supervision is actually being participated in an average of 6 times per year. It should be noted that there are certain times within our careers when more frequent sessions are required. These tend to be around transitions: for example, new graduates taking up their first role, or staff members taking on new roles.
What about time to participate in supervision?
Having permission to carry out sessions and be away from the workplace is important. Encouraging staff to take up this opportunity and not cancel or reschedule but to see the benefit of this for themselves and also their patients. Did you know if a staff member takes one hour out per month and works full time this equates to 1.6 % of their work time annually?
How are sessions structured?
Supervision sessions should be supervisee driven and based on a supervision agreement (see the supervision agreement example) where supervisor and supervisee agree on the focus of the sessions, goals for the sessions as well as practical considerations. Our workforce made the request that we developed a practical guide which could be easily implemented in practice and the Page and Wosket model (2014) was modified and used to outline how to prepare for supervision, what happens before, during and after.
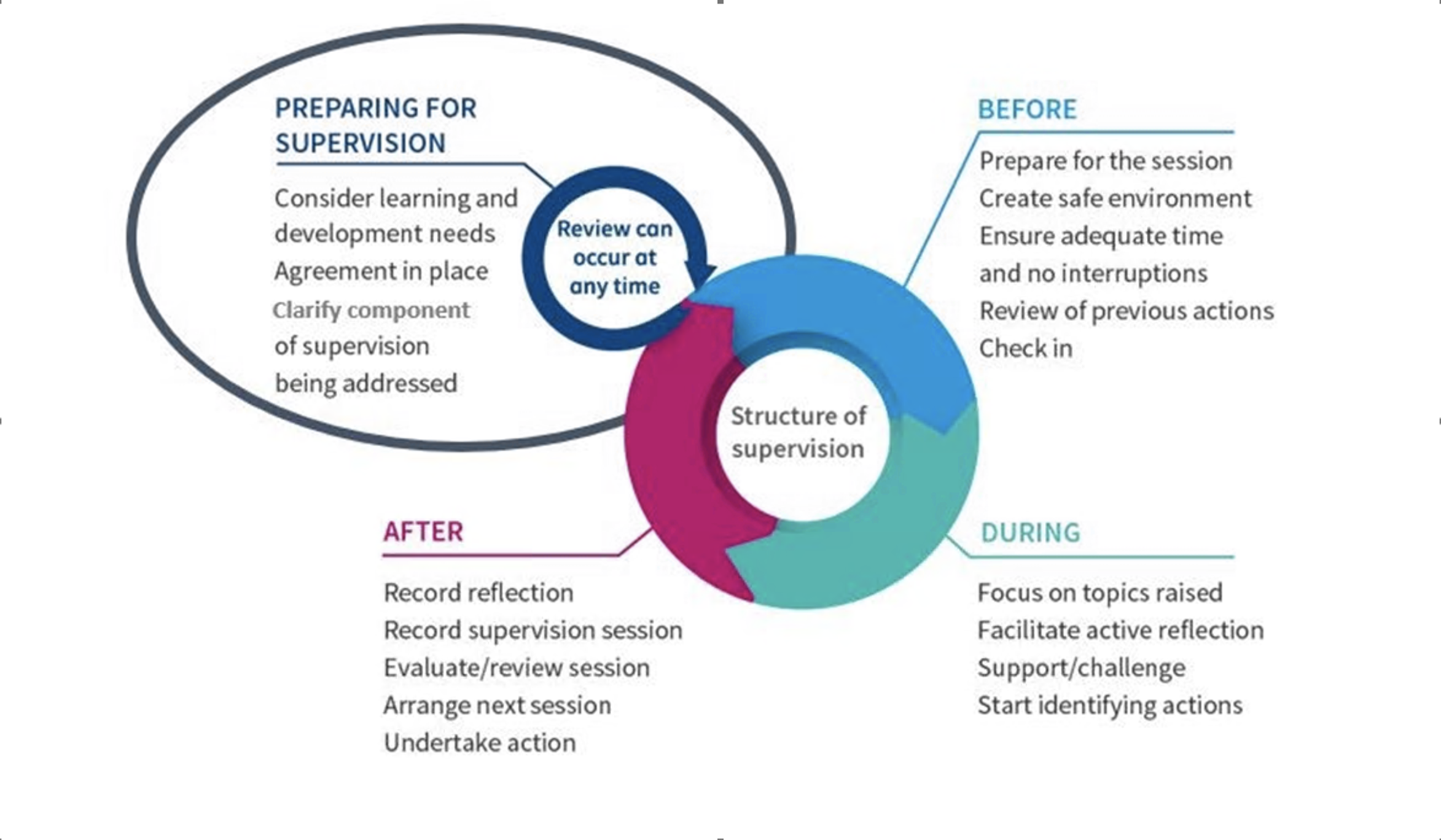
How do we record sessions?
Recording your session and keeping records is a joint responsibility. Supervisees should be encouraged to keep personal reflections on their learning from a supervision session and supervisors keep an aide memoir of issues raised/discussed. We are currently working on developing national guidance for recording and storing supervision records. (See the recording example.)
How can we evaluate supervision?
It is important to audit that not only is supervision taking place in your area but also the quality and effectiveness of it. This can be achieved in various ways for example at the end of each session, it is good practice to consider what went well within the session and if anything could have been improved. However, it is also important to have regular evaluation using the supervision agreement to ensure sessions remain focused and helpful. You may also wish to carry out a service wide evaluation to determine success of implementation of supervision within the workplace.
Where do employers / line managers get their practice / professional supervision from?
As we have already mentioned it is important that ALL AHP staff engage in regular and quality supervision – and this includes employers! Consider where you get you your own practice and professional supervision. You may need to make additional arrangements for yourself.
You can access a summary of the work to date and view the education resources developed to support supervision practice on Turas.
Article references
-
Allied Health Professions in Scotland (2018) Scotland’s position statement on supervision for allied health professions ( Download, 302 KB), NHS Education for Scotland, Edinburgh.
Andrews J, Butler M (2014) Trusted to Care. An independent Review of the Princess of Wales Hospital and Neath Port Talbot Hospital at Abertawe Bro Morgannwg University Health Board. Dementia Services Development Centre, University of Stirling. https://gov.wales/sites/default/files/publications/2019-04/trusted-to-care.pdf (Last accessed: 21st January 2022)
Chief Nursing Officer Department (CNOD)/Scottish Government (2017) Nursing 2030 Vision. Scottish Government, Edinburgh.
Department of Health (2012) Transforming care: A national response to Winterbourne View Hospital Department of Health Review: Final Report. DH, London.
HCPC: https://www.hcpc-uk.org/resources/reports/2019/effective-clinical-and-peer-supervision-report/
Kirkup B (2015) The Report of the Morecambe Bay Investigation. Stationery Office, London. https://www.gov.uk/government/publications/morecambe-bay-investigation-report (Last accessed: 21st January 2022)
NHS Education Scotland, Allied Health Professions Education Strategy: 2014-2020 (Last accessed: 21st January 2022)
NHS Education Scotland Strategy 2019-2024 https://www.nes.scot.nhs.uk/media/kacboen5/nes_strategic_framework_2019_2024.pdf (Last accessed: 21st January 2022)
NES Position Statement - Clinical Supervision: Nursing & Midwifery Workforce (Scotland) ( Download, 520 KB)
Nursing and Midwifery Council (NMC), (2019) Standards of Proficiency for Midwives https://www.nmc.org.uk/globalassets/sitedocuments/standards/standards-of-proficiency-for-midwives.pdf (Last accessed: 21st January 2022)
Nursing and Midwifery Council (NMC), (2018) Future Nurse: Standards of Proficiency https://www.nmc.org.uk/globalassets/sitedocuments/standards-of-proficiency/nurses/future-nurse-proficiencies.pdf (Last accessed: 21st January 2022)
Nursing and Midwifery Council (NMC), (2021) Principles of preceptorship https://www.nmc.org.uk/standards/guidance/preceptorship/ (Last accessed: 21st January 2022)
Proctor B (1987) Supervision: Proctor a co-operative exercise in accountability. In: Marken, M., Payne, M. Enabling and Ensuring: Supervision in Practice. National Youth Bureau and the Council for Education and Training in Youth and Community Work, Leister pp. 21-34; 1987
Rothwell.C, et al (2019) The characteristics of effective clinical and peer supervision in the workplace: a rapid evidence review, Health Care Professions Council and Newcastle University effective-clinical-and-peer-supervision-report.pdf (hcpc-uk.org) (Last accessed: 21st January 2022)
The Mid Staffordshire NHS Foundation Trust Public Inquiry (2013) Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry: executive summary. Stationery Office, London (Chair: R Francis). https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/279124/0947.pdf (Last accessed: 21st January 2022)
The Vale of Leven Hospital Inquiry (2014) The Vale of Leven Hospital Inquiry Report. Edinburgh (Chair: Lord McLean). https://hub.careinspectorate.com/media/1415/vale-of-leven-hospital-inquiry-report.pdf (Last accessed: 21st January 2022)
More resources for employers
Get updates relevant for employers of HCPC registrants delivered straight to your inbox
Subscribe to receive HCPC insights for employers by entering your email address below.
- Published:
- 07/10/2022
- Resources
- Learning material
- Subcategory:
- Information and support
- Audience
- Employers





