The levels of practice are a workforce development framework to describe stages within the broader health and care workforce
The levels of practice are not a regulatory requirement, and HCPC standards apply to registrants at all levels of practice. This page provides an overview of advanced levels of practice and how they support safe and effective professional practice that meets the needs of service users.
Defining advanced levels of practice
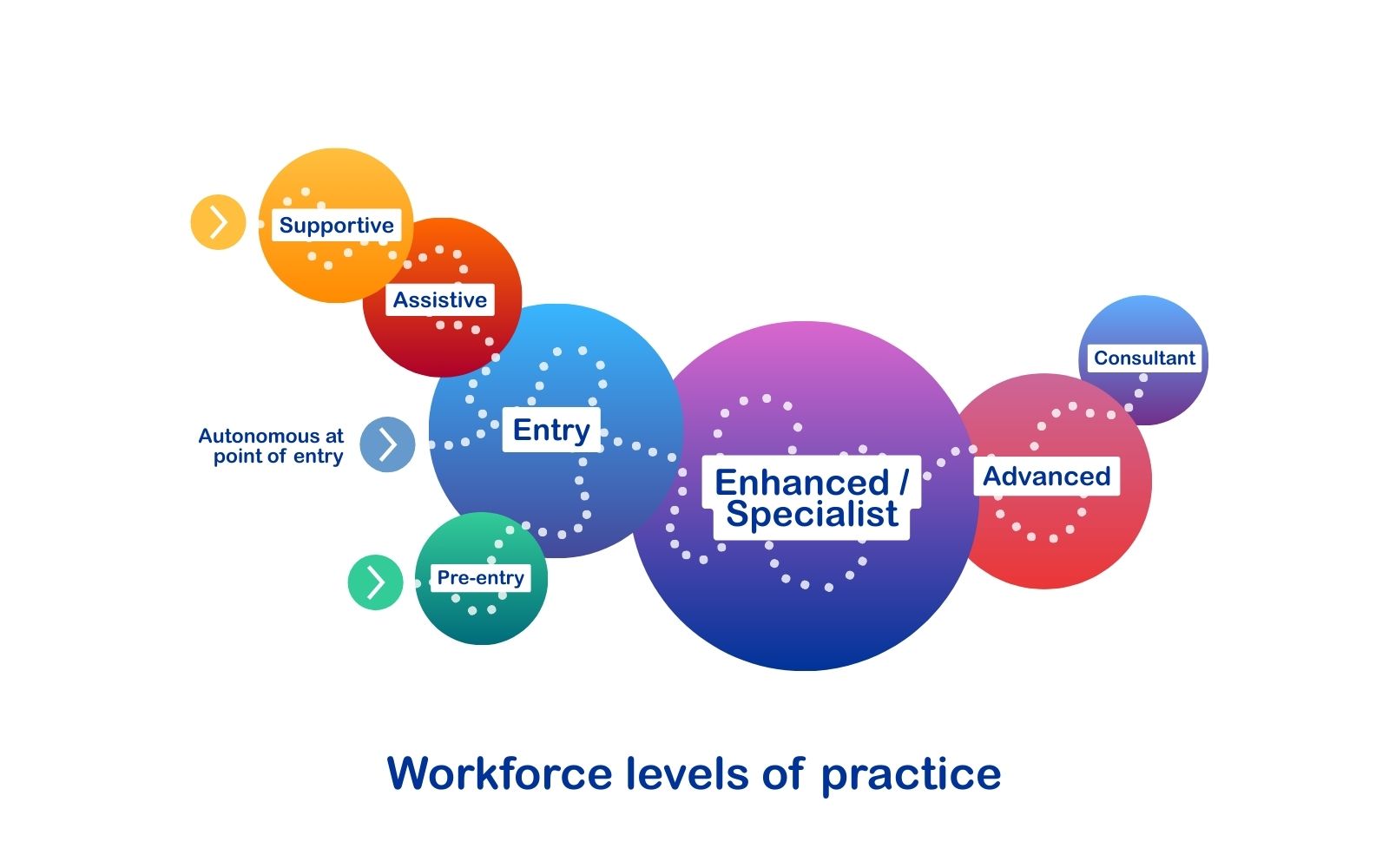
The three advanced levels of practice in the UK are:
- Enhanced (in England and Wales) or Specialist (in Northern Ireland and Scotland)
- Advanced
- Consultant
These build on previous levels of practice which are sometimes referred to as entry, foundation or newly qualified. There are many different roles and job titles across sectors at these levels of practice. Some roles remain within individual professions and some roles are multiprofessional.
HCPC registrants at all levels are fully regulated, and the levels of practice are not an HCPC regulatory requirement. The levels have been developed as part of ongoing work to provide clarity about career progression, and to support the education, training, governance and organisational oversight that is needed to support role development for experienced health and care professionals. They can support you to identify CPD opportunities as you consider ways to evolve your scope of practice to meet service user needs and to support service redesign.
The definitions originate in the national health sectors across the UK, so they may feel less familiar if you are working in roles across the broader health and care system in different sectors. However, the terminology, or variations of it, has been widely adopted in resources relevant to those working across all sectors for example in career development frameworks from professional bodies.
At the point of registration (Entry), you are expected to practise autonomously, exercising your own professional judgement to meet service user needs. With time, experience and, for some, additional qualifications, your level of autonomy may increase. For example, registrants working at the level of advanced practice are expected to exercise significant autonomy, judgement and responsibility in their roles.
At all levels of practice, any associated risks can be managed through a system-wide approach to safe and effective practice, which includes the existing regulatory arrangements. The HCPC continues to assess the risks in practice as part of our role to protect the public.
Determining your level of practice will require you to use your professional judgement to map your capabilities and your scope of practice against relevant professional and career development frameworks. There may be additional capabilities that require sign-off by some employers and with some roles too. At the advanced levels of practice, primarily for allied health professions, each UK country has its own publication to support you. Many professional bodies have published relevant resources too.
Common to many of the workforce development resources is the concept of the four pillars of practice. Working across all four pillars is not a regulatory requirement, but they can be used to define and explain your scope of practice and related CPD activities. Our advanced levels of practice FAQs and resources can also support you with this.
Four pillars of practice
There are four pillars of practice, which are sometimes called domains of practice in some professional body frameworks. There is a workforce expectation that individuals working at the level of advanced practice will work across all four pillars of practice:
- Clinical practice (or professional practice)
- Leadership and management
- Education and learning (or facilitating learning)
- Research and evidence (or evidence, research, and innovation/development)
These pillars represent the knowledge, skills and behaviours needed to:
- provide high-quality healthcare that is safe, effective and person‑centred (clinical practice);
- lead yourself and others and fulfil management and leadership responsibilities (leadership and management);
- enable effective learning for yourself and others in the workplace (education and learning); and
- engage in research activities and use the evidence to improve practice and services (research and evidence).
The ‘size’ of each pillar will vary according to your individual scope of practice and role(s). The pillars may go up or down as a proportion of your work-based activities depending on the nature of your career progression if, for example, you change roles, as shown in the illustrative examples.
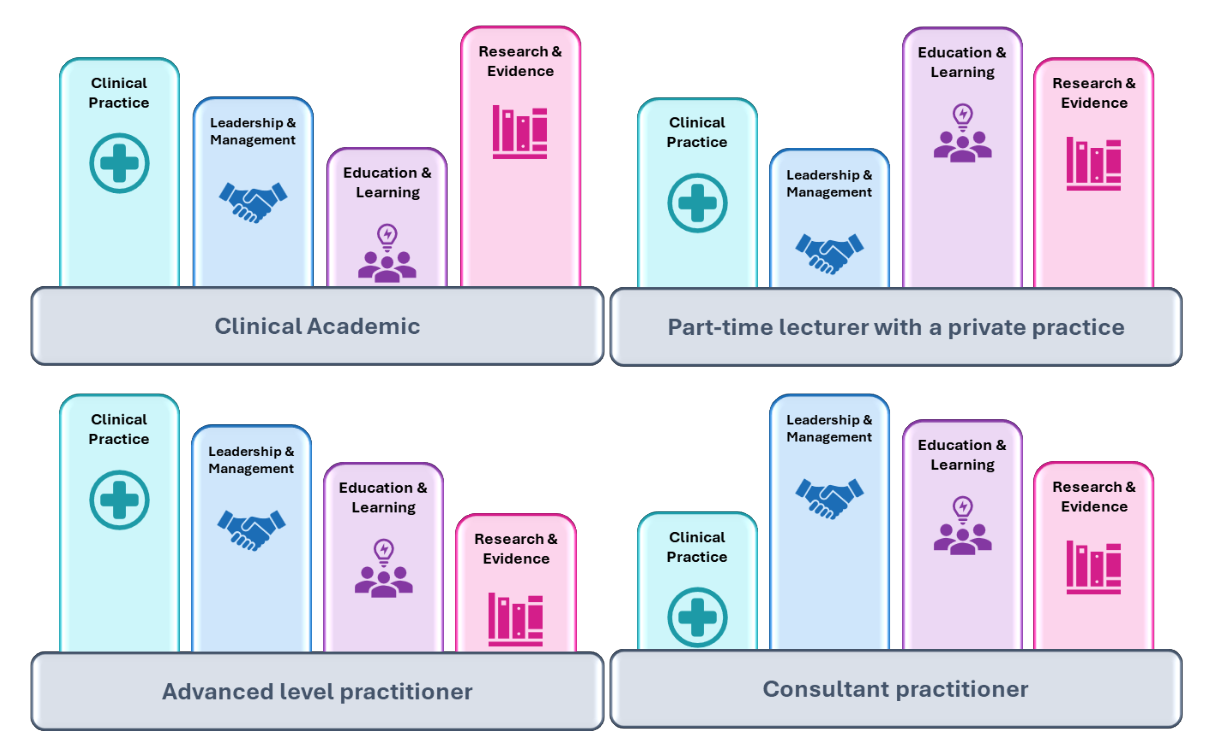
Job titles
There are a range of job titles across advanced levels of practice. While designated titles for each profession are protected by law, job titles are determined by the employing organisation and not the regulators. The titles, pay, terms and conditions vary across organisations.
The lack of clarity in the various titles can cause confusion for the public, especially when the protected title does not form part of the job title.
Efforts across the UK are seeking to provide clarity for registrants, managers and organisations about routes into different levels of practice, alongside the governance and oversight to support them. For example, work in Scotland has introduced a national job title format for NHS allied health professional advanced practice roles to provide greater clarity and consistency for the public and the wider workforce.
Your HCPC standards require you to work in the best interests of your service users and to communicate clearly and honestly with them at all times.
We encourage you to use job titles that help your service users to understand your knowledge, skills, and experience, and include your profession or protected title.
We recommend discussing any further questions about job titles with your employer and/or professional body.
Supporting advanced levels of practice: roles in the system
Statutory regulators, like the HCPC, are only one part of the system that supports advanced levels of practice. Safe and effective practice is a shared responsibility between the registrant, the regulators (including the system regulators), the employing organisation (where appropriate) and the professional body, all working together within a legal framework.
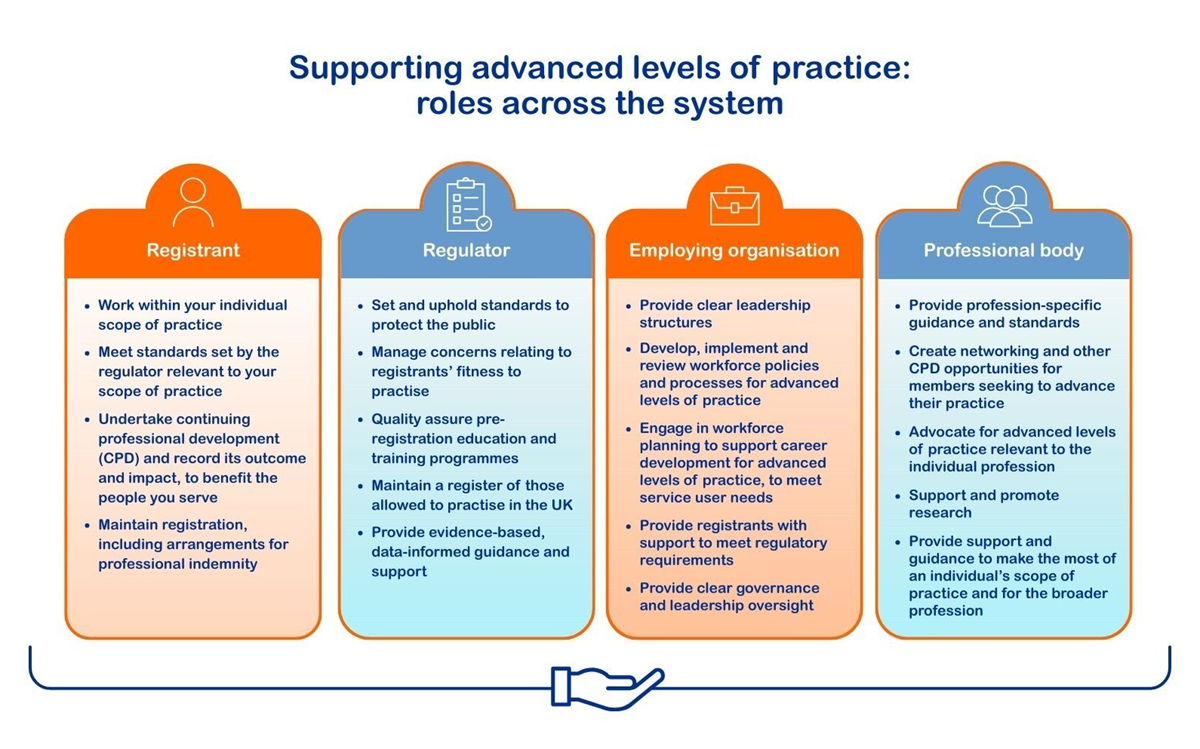
You can find more information about our role in supporting safe and effective practice at advanced levels on our Regulating advanced levels of practice page.
Glossary of key terms for advanced levels of practice
This is a list of frequently used terms in the discussions of advanced levels of practice. These terms have not been developed by a single regulator and remain agile as part of contemporary workforce development planning. Different UK nations may have their own definitions which respond to their individual workforce needs.
Expand all
-
ACP is one of many roles at the level of advanced practice. ACPs come from a range of HCPC-regulated and other professions including nursing, midwifery, osteopathy and pharmacy. Also see the term ‘advanced level’’ for a broad description of the knowledge, skills and experiences that underpin all roles at the advanced level of practice including ACP.
-
One of the advanced levels of practice, sitting between enhanced/specialist and consultant.
The following definition has been agreed across the four UK countries in the statement ‘Advanced practice in the Allied Health Professions (AHPs)’ to provide clarity about how advanced practice for AHPs is defined:
“Advanced practice in allied health professions involves complex decision making, underpinned by a post-registration master’s level award or equivalent undertaken by an experienced practitioner that encompasses all four pillars of practice: clinical practice, leadership and management, education, and research. It is delivered by skilled and experienced registered health and care professionals who exercise significant autonomy, judgement and responsibility in their roles.
Advanced practitioners manage complex care in partnership with individuals, families and carers, analysing and synthesising complex problems, often as part of multi-professional teams. They handle clinical risk and uncertainty across significant areas of work, in various settings, developing innovative solutions to expedite access to care, optimise peoples’ experiences, drive population health and prevention and improve outcomes.”
The term ‘advanced practice’ is not to be confused with the phrase ‘advanced levels of practice’, which refers to three levels of practice; enhanced/specialist, advanced and consultant.
-
The advanced levels of practice comprise three levels namely: enhanced / specialist, advanced and consultant. There are professional frameworks in place in each of the four UK nations to support the workforce development of the experienced workforce. The language differs slightly across the UK, for example, ‘specialist’ is used in Scotland and Northern Ireland, but in England and Wales, ‘enhanced’ is used to describe the same level of practice. There are a range of roles at each level (see also the term ‘levels of practice’).
-
AHPs is a classification used to describe a range of regulated professions who are regulated by the HCPC or the General Osteopathic Council (GOsC). The allied health professions include art therapists, dietitians, dramatherapists, music therapists, occupational therapists, operating department practitioners, orthoptists, paramedics, physiotherapists, podiatrists, prosthetists and orthotists, radiographers, and speech and language therapists. However, there are variations across the four UK countries, for example osteopaths are considered AHPs in England only and radiographers and operating department practitioners are considered healthcare scientists in Wales.
-
A career development framework is a structured system that maps how professionals can grow within their careers. Many professional bodies have profession-specific frameworks that outline the knowledge, skills and experiences which members, registrants and managers can use as part of planning continuing professional development activities. See also the term ‘four pillars of practice’.
-
A CAHPO holds office in each of the four UK nations. They act as the professional leader responsible for advising the governments on matters affecting AHPs. They oversee the strategic direction of the AHP professions, across all levels of practice, and they work closely with health and care regulators.
The equivalent of the CAHPOs for healthcare scientist professions is the Chief Scientific Officer.
-
The consultant level is the highest level within the workforce development structure, sitting above the levels of enhanced/specialist and advanced practice. While no centrally agreed definition exists across the four UK nations, professionals working at the consultant level of practice work across the four pillars of practice (sometimes referred to as domains) and provide consultancy. In England, the consultant level of practice includes:
- Expert practice: help firmly establish values-based professional practice across pathways, services, organisations and systems, working with individuals, families, carers, communities and others
- Strategic, enabling leadership: provide values-based leadership across the care pathway, services and systems in complex and changing situations
- Learning, developing and improving across the system: develop staff potential, add to, and transform the workforce, help people to learn, develop and improve (in and from practice) promote excellence
- Research and Innovation: develop a ‘knowledge-rich and inquiry’ culture across the service and system that contributes to research outputs driving positive impact on development and quality with regard to innovation and improving capability in staff and systems
- Consultancy across 1-4 across the system using consultancy approaches and opportunities that have maximum impact on practice, services, communities and populations, and which add to and sustain workforce capacity and capability
-
CPD is the way in which registrants continue to learn and develop throughout their careers, so that they keep their skills and knowledge up to date and are able to practise safely and effectively. The HCPC operates an outcome-focused CPD model, which means that activities are not prescribed nor is there a specified number of CPD hours or activities that registrants must complete. Registrants are required to maintain a record of their CPD activity, focusing on the outcome of their learning to benefit their individual service user groups. In some workplaces, registrants working at the level of advanced practice may be required by their employer to record their CPD activities as part of a professional portfolio.
-
Delegation involves asking someone to carry out an activity on your behalf. It involves assigning an activity to someone else who has the knowledge, skills and experience needed to carry it out safely and effectively. The person accepting the delegated activity must continue to be provided with appropriate supervision and support, which reinforces that delegation is a relational activity.
-
Enhanced practice is a level of practice defined as part of a workforce structure in England and Wales. In Scotland and Northern Ireland, the term ‘specialist’ is used to describe the same level of practice (see also the term ‘specialist level’). It sits below the advanced and consultant levels of practice. Professionals working at the level of enhanced practice will use a wide variety of job titles and are experienced registered professionals who undertake complex work and manage day to day risks. Like the other levels of advanced practice professionals working at the level of enhanced practice work in multiple settings.
Enhanced practice can be a precursor to advanced practice, or it can be a valued workplace destination in itself, offering services and service users a consistent level of expertise.
-
The Four pillars of practice are a workforce structure which encompass clinical practice, leadership and management, education, and research. The pillars have been adopted in many resources, including career development frameworks from professional bodies, for all career levels. There is a workforce expectation that professionals working at the levels of advanced and consultant practice work across all four pillars (see also the terms ‘consultant level’ and ‘advanced level’).
-
Governance arrangements are structures and processes that lead, direct, and control the quality of service. This may include identifying and minimising risks, ensuring required standards are achieved, and investigating sub-standard performance. Ways that they achieve this include mandatory training for staff, assessment of performance and sharing best practice. Governance arrangements are essential for ensuring the delivery of high-quality and sustainable health and care services.
-
Levels of practice are workforce structures and are not formal regulatory levels. Regulatory standards apply across all levels of practice for registrants (see also the term ‘advanced levels of practice’).
-
See the term ‘professional body’.
-
Multiprofessional / multidisciplinary refers to a collaborative approach where various health and care professionals work together to deliver high-quality care. Multiprofessional and multidisciplinary teams and environments emphasise the importance of flexibility, as well as the value of the distinct contributions of each professional. Multiprofessional approaches aim to enhance service user outcomes and improve the overall effectiveness of health and care delivery.
-
A professional body represents a profession and advocates its concerns and interests. Membership or professional bodies often will be involved in safeguarding standards and promoting good practice, but they are not regulators and do not hold a statutory (legal) function.
-
Registrants are required to have a professional indemnity arrangement in place as a condition of registration with the HCPC. The arrangement must provide cover appropriate to a registrant’s practice, taking into account the nature and extent of its risks. It will need to be sufficient to meet any liability that may be incurred if a successful claim is brought against you. For further information, visit the HCPC webpages.
-
Professional judgement involves the use of accumulated knowledge and experience, as well as critical reasoning, to make an informed professional decision in the specific context of the situation. The ability to use professional judgement to apply the HCPC’s standards and work in the best interest of service users is an essential part of being an autonomous professional.
-
A registrant is an individual who is currently on the Register of the relevant regulator for their profession, in this case, the HCPC.
-
The primary aim of a regulator is to protect the public. The HCPC is a statutory regulator which carries out legal functions relating to a profession (or professions). HCPC regulates 15 health and care professions in the UK and protects the public by setting standards for professionals’ education and training and practice, approving programmes which professionals must complete to register with the regulator, keeping a register of professionals (known as registrants) who meet the standards and taking action if professionals on the Register to not meet the standards.
-
Regulatory standards are expectations set by regulators, like the HCPC, that regulated individuals must meet. Regulatory standards sit alongside laws and other guidelines to ensure safe and effective practice. HCPC standards include:
The standards of proficiency: These set clear expectations of registrants’ knowledge and abilities when they start practising, and all registrants must meet these standards to join the HCPC Register. Once on the Register, registrants must continue to meet the standards of proficiency that apply to their scope of practice.
The standards of conduct, performance and ethics: These set out expectations for registrants’ behaviour and what the public can expect from a health and care professional, and are the ethical framework within which all registrants must work. These standards help to inform decisions about the character of professionals who apply to the HCPC Register, and are used when a concern is raised about a registrants’ practice.
The standards of continuing professional development: These set expectations around demonstrating continuing learning and development. Registrants must meet these standards when undertaking CPD activities, and are used when a CPD audit is undertaken.
The standards relevant to education and training: These set expectations for how education and training programmes should prepare learners for professional practice. These standards are used to assess education and training programmes and approve suitable programmes to give successful graduates eligibility to apply to the HCPC Register.
-
Scope of practice is the area or areas where a professional has the knowledge, skills and experience to practise lawfully, safely and effectively, in a way that meets the standards and does not pose any danger to the public or to themselves. An individual’s scope of practice is likely to change over time with additional knowledge, skills, and experience, and for some, additional qualifications.
Scope of practice is a living process comprising two inter-related elements: individual and profession. Both evolve and change over time. An individual’s scope of practice may extend beyond the generally accepted boundaries of the origin profession with appropriate experience, education, training and organisational oversight.
Any change in a scope of practice must be to effectively meet service user needs and be done so with organisational oversight and governance (where appropriate).
-
Scope optimisation involves identifying ways to make the best use of the whole workforce at all levels of practice, in terms of their time, knowledge and skills to benefit service users. Scope optimisation can be realised through effective delegation across the entire workforce (including delegating to the support workforce).
-
The term encompasses all the areas where registrants work including public sector health and care settings, academic institutions, third sector, private sector and many more.
-
Service user is a broad phrase that refers to anyone who uses or are affected by the services of professionals registered with the HCPC. This can include patients, families, carers, students and learners, colleagues, people who are line-managed by a registrant and more.
-
Specialist practice is a level of practice defined as part of a workforce structure in Scotland and Northern Ireland. In England and Wales, the term ‘enhanced’ is used to describe the same level of practice (see also the term ‘enhanced level’). It sits below the advanced and consultant levels of practice. Professionals working at the level of specialist practice will use a wide variety of job titles and are experienced registered professionals who undertake complex work and manage day to day risks. Like the other levels of advanced practice professionals working at the level of specialist practice work in multiple settings.
The level of specialist practice can be a precursor to advanced practice, or it can be a valued workplace destination in itself, offering services and service users a consistent level of expertise.
-
Supervision is a core component to maintain safe and effective practice in all sectors and settings. It is a process of professional learning and development that enables individuals to reflect on and develop their knowledge and skills through agreed and regular support with another professional.
-
System-wide refers to an approach that happens across an entire system rather than in individual settings or sectors. It signifies that changes, policies or effects are applicable and relevant throughout every component of a system.
-
The word title may refer to the job title of a particular role, or the designated titles for professions which are protected by law. Protected titles are the designated titles that professionals are only entitled to use while practising in the UK if they are on the relevant register held by a statutory regulator, like the HCPC. The HCPC regulates protected titles for 15 professions.
Job titles are set by employing organisations and can vary between sectors and organisations. These titles may include the designated/protected title of your profession and your level of practice. Apart from the use of protected titles, the regulator does not set or limit the titles a professional may work under.
Related content
Multi professional resources
- In England, the Centre for Advancing Practice has a number of resources for the enhanced, advanced and consultant levels of practice, including capability frameworks, principles and guidance for supervision and case studies, featuring practitioners at the advanced levels of practice.
- The NHS Scotland learning platform Turas has a dedicated Advanced practice toolkit. Resources include rural workplace supervision, learning across the four pillars of practice, and examples from practice. The Nursing, midwifery and allied health professionals (NMAHP) development framework offers a structured way to identify post-registration CPD opportunities
- Health Education and Improvement Wales has published a professional framework for enhanced, advanced and consultant clinical practice.
- The Department of Health Northern Ireland has published the Advanced AHP practice framework.
- There are also resources that focus on individual pillars of practice such as the Council of Deans for Health AHP Educator Career Framework and the NHS England Multi-professional practice-based research capabilities framework.
- These are examples of a larger library of resources, including those from professional bodies, that can support registrants to identify their level of practice and areas for CPD to continue to appropriately grow their scope of practice.



